How to Reduce Excess RhIG Usage in Your Practice
DOWNLOAD A FREE COPY OF THE 2015 STUDY
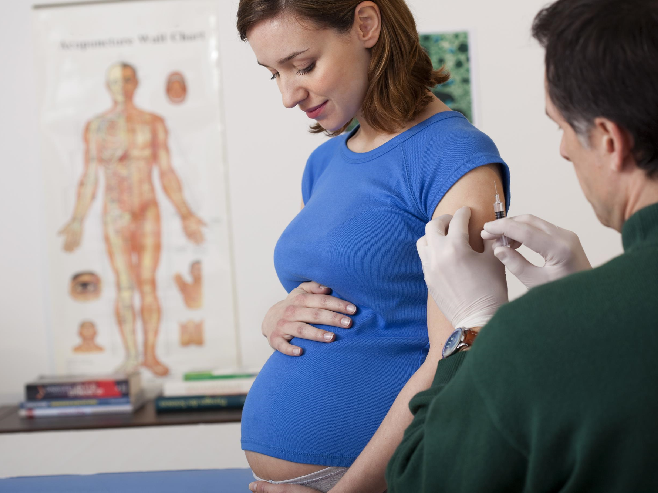
Rh immune globulin (RhIG), composed of RhD antibodies, prevents a patient’s immune system from mounting a response to the RhD antigen. Physicians routinely administer RhIG for several purposes, but most often for prevention of alloimmunization in RhD-negative pregnant women.
However, when RhIG is administered unnecessarily, it carries ethical implications. RHD genotyping can accurately classify a patient’s RhD status in cases where traditional serologic testing cannot, and the result can be reducing excess usage of RhIG in clinical practice.
The Purpose of RhIG
A mother is at risk of RhD alloimmunization if she is RhD negative and her fetus is RhD positive. Alloimmunization generally doesn’t affect the first pregnancy; however, in subsequent pregnancies, maternal antibodies can cause hemolytic disease of the fetus/newborn (HDFN), which can be fatal to the fetus. The American Journal of Obstetrics and Gynecology reports that in countries without RhIG protocols, up to 14 percent of affected fetuses are stillborn.
The American College of Obstetricians and Gynecologists (ACOG) recommends that all RhD-negative mothers receive RhIG around the 28th week of pregnancy, as alloimmunization to the RhD antigen would typically occur after this. It also recommends the mother receive another dose of RhIG within three days of delivery of an RhD positive neonate.
Excess Use of RhIG
The testing of expectant mothers to determine their RhD status has been standard practice for decades, but serologic RhD testing results aren’t always definitive or consistent. RHD gene variants may cause expression of a variant RhD antigen on red cells. Many times, these variants are recognized as serologic weak D phenotypes, where red blood cells initially react weakly (<2+) with RhD reagent antibodies, but react moderately or strongly with the addition of antihuman globulin.
Patients with serologic weak D phenotypes are often managed conservatively, as RhD-negative, although those with Weak D Types 1, 2 or 3 can be safely managed as RhD-positive. On the other hand, individuals with RHD variant genes other than Weak D Types 1, 2 or 3, including those with partial D variants are at risk for clinically significant sensitization, should be treated as RhD-negative for transfusion and are candidates for Rh immune globulin.
The primary ethical implication of unnecessary RhIG injections is that RhIG is obtained from RhD-negative male donors, who must be intentionally alloimmunized to produce RhD antibodies. The costs of RhIG therapy, including paying donors, manufacturing, shipping, storing and administering the drug, in addition to the patient testing required, make its unnecessary use an ethical concern as well. A human-derived product like RhIG should only be used for patients who really need it.
Benefits of RHD Genotyping
Accurate RhD blood typing is important for the clinical management of obstetrics patients and for transfusion recipients. Fortunately, RHD genotyping can accurately identify RHD variant genes and guide proper patient management when serologic tests are not definitive. The College of American Pathologists (CAP) and American Association of Blood Banks (AABB) convened a Work Group to develop recommendations for implementing RHD genotyping to maximize its benefits, such as eliminating unneeded injections of RhIG. The Work Group recommended RHD genotyping for obstetrics patients and transfusion recipients with a serologic weak D phenotype or discordant RhD typing results.
A 2015 publication by Sandler et al. estimated that of 16,700 obstetrics patients with serologic weak D phenotypes annually, approximately 13,360 would be Weak D Types 1, 2 or 3, and could be managed as RhD positive. Identifying these patients with RHD genotyping would prevent the unnecessary administration of an estimated 24,700 injections of RhIG every year in the United States.
RHD genotyping of transfusion recipients with serologic weak D phenotypes is also advantageous, as an estimated 21,900 individuals with serologic weak D phenotypes are transfused annually. RHD genotyping would identify approximately 17,520 of these patients as Weak D Types 1, 2, or 3, who could receive RhD positive blood for transfusion. Considering an average of 2.7 units per transfusion, identifying these patients with RHD genotyping would preserve 47,700 RhD-negative units for patients who really need them.
Excess RhIG usage is not only costly but also carries ethical implications. RHD genotyping reduces unnecessary injections of the drug while also standardizing and improving the quality of care for obstetrics patients. For more on the procedure and tips for phasing it in at your practice, download a copy of “It’s time to phase in RHD genotyping for patients with a serologic weak D phenotype” by Sandler et al. (2015) here.
